Hope you enjoy!
In her Honor
I have traveled to twenty-six countries on five different continents. I have found myself delivering babies by candlelight, wrapping newborns in pieces of old cloth, and sterilizing my instruments in boiling water. I have operated on women’s prolapsed uteri from which they had suffered in silence for years. I have done PAP smears on women never before screened for cervical cancer; and performed surgical excisional procedures for those harboring pre-cancerous lesions. So, by the age of thirty, I thought I understood the hardships of the world.
However, working in the labor and delivery unit at the largest national referral hospital in Kampala, Uganda, revealed to me I had much to learn about the consequences of poverty.
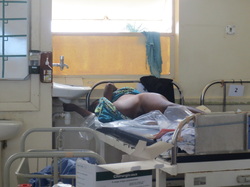
The sound echoing from that room was one I had never heard. Was it the beeping sound of fetal heart rate monitors or the whirl of epidural pumps? No; the only sound was of thirty-five women moaning and groaning to the pains of childbirth. Laboring women covered the ground, their amniotic juices and bright red blood saturating the plastic tarps spread to protect the floor.
Midwives were hard at work but none were smiling. They seemed defeated by the number of patients and the lack of access to necessary life saving resources. Desperation radiated from every laboring woman's face, each pair of eyes sent a silent plea to allow her and her unborn child to survive the journey.
On my first day, still in shock from the sights and sounds, I patiently coached a new mom in the birth to her daughter. After her perfect little being was born, the mother asked me my name.
"Karina", I responded. She looked down at her precious newborn and said "So is hers". I was not prepared for the extreme contradictions before me; I was moved by this mother’s choice and the beauty of a healthy birth, yet, I was also aware that we were surrounded by serious complications, limited resources, preventable tragedies, and overwhelming desperation.
I went to Mulago Hospital with the intention of being an observer. I had a professional interest in how obstetrical and gynecological care differed in a low-income country from my practice in the United States. I wanted to understand why one in every 12 women in this country had to die in childbirth, and hoped to identify ways the willing hands of American physicians might help minimize the current inequalities in medical care. However, as I saw what was happening and witnessed the dire need of a competent health care provider, it was impossible to stand on the sideline. I couldn't let the woman in front of me suffer from an obstetrical emergency if I had the ability to perform the necessary surgery. I felt compelled to engage and I did.
I will never forget Mrs. Palasco, mother of seven, who arrived to the hospital seizing from eclampsia. I took a deep sigh of relief when I found a reassuring fetal heart rate but the mom was clearly unstable. We had to stabilize the patient before doing a cesearean to save the baby. It took me fifteen minutes to locate a functioning blood pressure cuff and another ten minutes to find a working pulse oximeter. I immediately ordered magnesium sulfate to protect the mom from having a stroke, but it arrived more than hour later.
Meanwhile, the patient continued to convulse. Her blood pressure was severely elevated but there were no available anti-hypertensive in the hospital pharmacy. The family dug through their satchels but couldn’t gather enough money to purchase the necessary medication. I handed the son a few dollars from my own purse and he sprinted out of the hospital in search of this life saving remedy. Finally, we got the blood pressure out of a dangerous range, her seizures stopped, and thankfully, there was still a fetal heart. The patient was ready for surgery. But, as always, there was a long line of extremely sick women waiting for a cesarean section and the patient with immediate life-threatening issues took precedence. A patient with a ruptured uterus was taken back to the operating room, followed by a women and fetus suffering from a cord prolapse. The emergencies never stop. Twelve-hours later, I finally performed a cesarean section on Mrs. Palasco. I delivered an alive but struggling baby boy. Mrs Palasco never opened her eyes to see her newborn child; she died from a hemorrhagic stroke that occurred as she waited for treatment.
In a country like Uganda, misery comes in many guises: lack of medications, lack of anesthesia or mandatory operating equipment. At other times it's the inability to efficiently monitor vital signs or because there just aren't available physicians. Mulago hospital has fifteen hundred beds but its average occupancy is greater than four thousand. Neither the thirty Ugandan house staff obstetricians nor the hospital resources can keep up with the overwhelming number of acute emergencies. I learned that the complexity of the many chains of causation are hard enough to comprehend let alone interrupt. I quickly realized that easy solutions simply do not exist for complex problems.
As an individual, I was overwhelmed when facing the enormity of the inequities and sufferings of Ugandan women, but I was comforted remembering that we are all part of something bigger than ourselves. As such, when we have the opportunity to take the first steps in being the change we want to see in the world we should take them. Hopefully, others will see the impact we are capable of creating for those left fortunate, and join the journey towards positive change.
